Brain cancer immunotherapy in mice more effective with drug coating
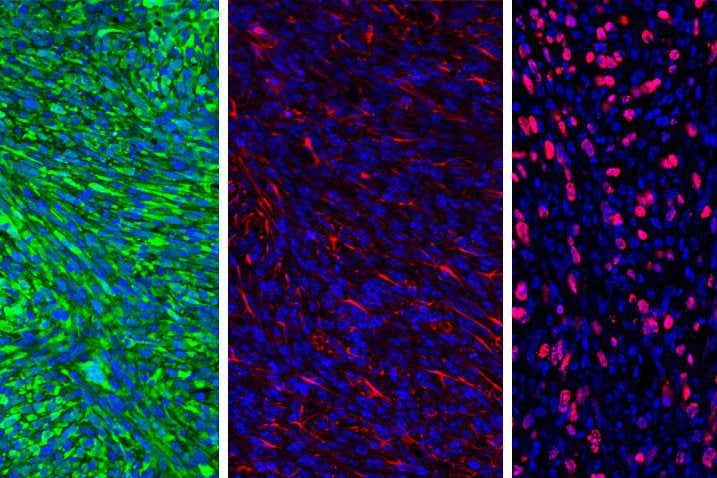
A nanoparticle coat helps an immunotherapy drug cross the blood-brain barrier in mice so it can target brain tumours more effectively
Health
26 May 2022
By Carissa Wong
Brain tumour cells University of Michigan Rogel Cancer Center
Coating a cancer drug with nanoparticles can help it cross the barrier that protects the brain from chemicals elsewhere in the body, enabling it to unleash an immune response that kills brain tumour cells. In a small study in mice, the encapsulated drug – used in combination with radiotherapy – eliminated tumours in 67 per cent of the animals.
Glioblastoma is an aggressive type of tumour that forms when brain cells called glial cells grow out of control. The condition makes up around a third of brain tumour cases, and has a very poor prognosis, with just 5 per cent of people surviving for 5 years after diagnosis.
These tumours are usually treated with surgery, followed by radiotherapy, and sometimes chemotherapy. However, while some drugs have shown promise at boosting the body’s immune response against brain tumours, the drugs often struggle to cross the blood-brain barrier to reach the tumour cells.
“These drugs, up until now, had been ineffective, as they could not penetrate the blood-brain barrier,” says Maria Castro at the University of Michigan Medical School.
Castro and her colleagues have now tested whether encapsulating a drug in synthetic nanoparticles – made out of proteins naturally found in the body – could help it reach the brains of mice. The team injected mice with either a drug alone or a nanoparticle-coated version. Eight hours later, mice that received the coated treatment had three times more of the drug in their brains than mice given a normal dose.
“This is a critical finding that will enable the development and implementation of novel therapeutic strategies for glioblastoma, as it enables effective delivery of drugs to the tumour,” says Castro.
Castro’s team then tested how well the drug – with and without the nanoparticle coating – worked in mice that had tumour cells implanted into their brains. Mice that received the encapsulated drug survived for 61 days, on average, after tumour cells were first implanted in their brains. The mice that received the drug alone survived for 45 days. Studying the brains of these mice revealed that the drug boosted the ability of immune cells to kill the cancer.
What’s more, the team found that a combination of the nanoparticle-coated drug and radiotherapy eliminated tumours in 67 per cent of mice, enabling them to survive for 90 days, on average, from the moment tumour cells were first implanted. In contrast, all mice that received either radiotherapy or the encapsulated drug alone had died after about 60 days. Mice that received standard radiotherapy treatment and no drug had the lowest survival rate – an average of 28 days.
“[The nanoparticle-coated drug] enhances the efficacy of radiation therapy, which is the standard of care for glioblastoma in human patients,” says Castro.
In a further experiment, the team implanted another batch of tumour cells into the brains of mice that had previously received the combination treatment. This revealed that these mice showed some immunity to the new brain cancer cells, suggesting that the therapy could act like a vaccine.
The treatment still needs to be tested to see if it works in other animal models of glioblastoma, before it could eventually be tested in humans.
“We envisage that this approach will be translated to the clinic within the next couple of years,” says Castro.
Journal reference: ACS Nanotechnology, DOI: 10.1021/acsnano.1c07492
Sign up to our free Health Check newsletter that gives you the health, diet and fitness news you can trust, every Saturday
More on these topics:
